Comprehending Perioperative Tachycardia
Comprehending Perioperative Tachycardia
Blog Article
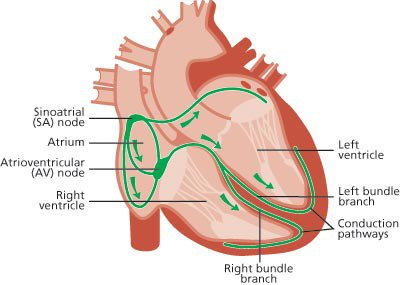
Perioperative tachycardia, a common occurrence throughout surgical procedures and the immediate following period, presents a issue for healthcare professionals. It refers to a rapid heart rate above a predetermined threshold, typically considered 100 beats per minute or more. This condition can arise as a result of a variety of factors, such as physiological stress, anxiety, pain, and underlying medical conditions. Understanding the causes and potential implications of perioperative tachycardia is crucial for providing optimal patient care.
Prompt identification and management are critical to minimize risks. Healthcare providers should closely monitor patients' heart rates during the perioperative period and implement appropriate interventions, such as fluid management, to restore hemodynamic stability.
Managing Postoperative Tachycardia: A Clinical Guide
Postoperative tachycardia, a common complication following surgery, can present significant challenges for clinicians. This syndrome is characterized by an elevated heart rate that typically continues for a prolonged period post-procedure.
Understanding the underlying mechanisms of postoperative tachycardia is crucial for developing effective management strategies. Various factors can contribute to this occurrence, including pain, anxiety, fluid depletion, and autonomic dysregulation.
Effective treatment of postoperative tachycardia entails a multimodal approach. Pharmacological often play a key role, with options such as beta-blockers and calcium channel blockers being to regulate heart rate. Alongside medication therapy, non-pharmacological can be beneficial. These may include stress reduction techniques, optimization of pain management, and appropriate fluid resuscitation.
A comprehensive assessment of the patient's clinical status, such as their medical history, current medications, and postoperative course, is essential for personalizing the management plan. Regular monitoring of vital signs, including heart rate, blood pressure, and oxygen saturation, is crucial to guarantee patient safety and optimally manage postoperative tachycardia.
Perioperative Heart Rate Elevation: Causes and Considerations
Elevated heart rhythms during the perioperative period can manifest as a common physiological response to various factors. A myriad of contributors can contribute this phenomenon, ranging from anesthetic agents and procedural stress to underlying medical conditions.
It's critical for clinicians to thoroughly determine the etiology of perioperative heart rate elevation, as it can affect patient outcomes and guide management strategies. A comprehensive evaluation should include a detailed review of the patient's medical history, baseline vital signs, and current medications.
Additionally, neurological examination findings can provide valuable clues regarding potential underlying conditions.
Is Tachycardia After Surgery Normal? Exploring Common Causes
Following a surgical procedure, the patient's heart rate may sometimes increase. This accelerated heartbeat, known as tachycardia, can be an expected occurrence in the postoperative period. It is important to note, understanding the underlying causes of tachycardia after surgery is important for accurate diagnosis and treatment. Some typical culprits include pain, anxiety, dehydration, medications, and anemia. Often cases, tachycardia resolves on its own as the body recovers.
However, if you are feeling persistent or intense tachycardia after surgery, it's vital to consult with your healthcare provider immediately.
The Incidence and Impact of Perioperative Tachycardia
Perioperative tachycardia occurs in a significant proportion of patients undergoing surgical procedures. This condition, characterized by an elevated heart rate prior to causes of tachycardia during surgery surgery, can have a detrimental impact on patient outcomes. The exact incidence of perioperative tachycardia varies depending on factors such as the type of surgery, anesthetic techniques employed, and the patient's underlying surgical conditions.
Increased heart rates can worsen hemodynamic instability, leading to complications such as hypotension, arrhythmias, and myocardial ischemia. Furthermore, perioperative tachycardia has been associated with an increased risk of postoperative mortality.
Recognizing the potential consequences, clinicians must actively monitor heart rate during the perioperative period and implement strategies to control tachycardia when required.
Tachycardia in the Operating Room: Assessment and Management
Tachycardia within the operating room can represent a significant hemodynamic issue. A rapid heart frequency necessitates prompt evaluation and effective management to maintain patient safety.
The initial step involves a thorough physical examination, including monitoring vital signs including heart rhythm, blood force, and respiratory effort.
A detailed history of the patient's preoperative medical condition should furthermore be obtained to determine potential contributing factors.
Electrocardiography is essential to establish the nature of tachycardia and detect any irregularities.
Blood tests may serve useful in evaluating electrolyte variations, thyroid status, and other variables that could be influencing to the tachycardia.
Based on the evaluation, management strategies should be adjusted to the underlying cause and the patient's overall condition.
Therapy options may include fluid administration, electrolyte adjustment, medication use to control heart rate and rhythm, and in some cases, urgent procedures such as synchronized cardioversion.
Continuous surveillance of the patient's vital signs and response to treatment is crucial throughout the perioperative period.
Factors Influencing Perioperative Heart Rate Dynamics
Perioperative heart rate variations are significantly influenced by a complex interplay of biologic factors. Preoperative patient characteristics such as age, underlying medical conditions, and anxiety levels can contribute to resting pulse. Intraoperatively, anesthetic agents, surgical stimulation, and hemodynamic adjustments can modulate heart rate. Postoperatively, pain, inflammation, and recovery processes also play a role in heart rate variability. Careful monitoring and intervention of these factors are crucial to ensure optimal cardiovascular outcomes during the perioperative period.
Postoperative Cardiac Acceleration
Post-operative tachycardia, characterized by an accelerated heart rate following surgery, can significantly/noticeably/potentially impact patient recovery. This condition can manifest as a result of various factors, including anesthesia, pain, and inflammation. While often temporary, persistent tachycardia may indicate/suggest/point to underlying complications, necessitating prompt/timely/immediate medical attention. Monitoring heart rate closely after surgery is crucial/essential/vital to ensure optimal healing and minimize potential risks associated with this common/frequent/usual postoperative phenomenon.
Perioperative Arrhythmias: Recognizing and Addressing Tachycardia
During the perioperative period, patients are prone to developing arrhythmias. One of the most common types is tachycardia, characterized by a heart rate above normal limits. Prompt recognition and management of tachycardia are crucial to patient safety. Symptomatic signs present with palpitations, shortness of breath, chest pain, dizziness, or fainting. An electrocardiogram (ECG) is the primary tool for diagnosing tachycardia. Treatment approaches depend on the origin and severity of the arrhythmia. Medications options include beta-blockers, calcium channel blockers, and antiarrhythmic agents.
In some cases, interventional procedures such as cardioversion or catheter ablation may be required.
Strategies for Minimizing Perioperative Tachycardia
Minimizing perioperative tachycardia demands a multifaceted approach that encompasses various pre-, intra-, and postoperative interventions.
A comprehensive assessment of the patient's medical history, including underlying conditions and medications, is crucial for identifying potential risk factors contributing to tachycardia.
Preoperative optimization strategies such as judicious fluid management, electrolyte balance correction, and anxiolysis can help mitigate autonomic response.
During surgery, attenuating the hemodynamic stress response through careful anesthetic techniques, adequate analgesia, and temperature control is essential. Maintaining a calm and supportive environment for the patient can also contribute to minimizing tachycardia.
Postoperatively, vigilant monitoring, early ambulation, and pain management are vital in facilitating recovery and preventing post-operative complications.
Monitoring Heart Rate Variability in the Operating Room: A Window into Surgical Stress
During surgical procedures, patients often experience physiological strain. This can lead to alterations in various bodily functions, including heart rate variability (HRV). HRV, a measure of the difference in time between consecutive heartbeats, provides valuable insights into the autonomic nervous system's response. Reduced HRV during surgery has been linked with increased risk of complications.
Physicians and researchers utilize HRV monitoring as a potential tool to assess cardiac performance during surgery. By analyzing the patterns of HRV, clinicians can gain a better understanding of the patient's physiological state. This information can be instrumental in modifying surgical strategies and ensuring optimal patient well-being.
- Furthermore, HRV monitoring may serve as an early warning of impending cardiac concerns during surgery, allowing for timely response to mitigate potential risks.
- However, the relationship between HRV and surgical stress is complex, requiring further investigation to fully elucidate its implications in clinical practice.
Anesthesia's Impact on Perioperative Tachycardia Management
Perioperative tachycardia presents a common challenge for anesthesiologists. Prompt and effective control is crucial to minimize adverse outcomes and ensure patient well-being. Anesthesiologists utilize a variety of techniques, including pharmacologic agents like calcium channel blockers, to regulate heart rate during both the induction and maintenance phases of anesthesia. Furthermore, optimizing anesthetic depth and monitoring hemodynamics closely are essential components of tachycardia suppression. By implementing these strategies, anesthesiologists can effectively manage perioperative tachycardia and contribute to a successful surgical outcome.
Preoperative Risk Factors for Postoperative Tachycardia
Identifying individuals at risk for postoperative tachycardia is crucial for optimizing perioperative care. Several preoperative variables can contribute to this issue. Elevated age is a significant risk factor, as the cardiovascular system may present greater stress during and after surgery. Pre-existing conditions such as hypertension, diabetes mellitus, and coronary artery disease can furthermore amplify the probability of postoperative tachycardia. Furthermore, certain anesthetic agents and surgical procedures inherently carry a risk for tachycardia.
- Intraoperative medication use, particularly beta-blockers or anticholinergics, can also influence the risk of postoperative tachycardia. Patients who are smokers may be more susceptible to this issue due to nicotine's effects on heart rate and rhythm.
Preemptive Treatment Strategies for Perioperative Arrhythmias
Perioperative tachycardia, a common cardiovascular complication during surgical procedures, can have adverse consequences for patient outcomes. Prompt detection and intervention are crucial to reduce the risk of complications like myocardial ischemia, arrhythmias, and hemodynamic instability. Medical professionals should implement a multi-pronged approach that includes continuous cardiac monitoring, meticulous intraoperative management, and appropriate pharmacological interventions. Moreover, patient education regarding preoperative risk factors and strategies to enhance cardiovascular health can contribute to a safer surgical experience.
Optimizing Fluid Management to Prevent Tachycardia After Surgery
Maintaining hemodynamic stability after surgery is crucial for patient recovery. One key aspect of this management involves optimizing fluid administration to prevent tachycardia. significant fluid shifts can trigger an rise in heart rate, potentially leading to complications. Therefore, meticulous monitoring of fluid input and output is essential. A balanced approach, considering factors such as patient age, pre-operative status, and surgical procedure, will help clinicians achieve appropriate hydration levels. Close collaboration between the anesthesia team and the surgical team is essential to execute a tailored fluid management strategy that minimizes the risk of postoperative tachycardia.
Perioperative Tachycardia: Effect on Surgical Outcomes
Perioperative tachycardia, a common physiological response during surgical procedures, has been associated to potential unfavorable outcomes. While some degree of tachycardia is anticipated in the perioperative period, significant elevations in heart rate can worsen various surgical issues. Studies have demonstrated a correlation between perioperative tachycardia and increased probability of postoperative complications such as wound infection, cardiovascular events, and prolonged hospital stay.
The underlying causes contributing to perioperative tachycardia are multifactorial and can include anesthetic agents, pain, stress, hypoxia, and autonomic nervous system imbalance. Identifying patients at high risk for perioperative tachycardia is crucial for implementing appropriate strategies to mitigate its potential adverse implications. Early detection and management of tachycardia can improve surgical outcomes, reduce postoperative morbidity, and enhance patient safety.
Patient-Specific Factors Influencing Postoperative Heart Rate
A multitude of unique factors can significantly influence postoperative heart rate. These factors encompass years of life, preexisting medical conditions, and pharmacological interventions the patient is receiving. Additionally, psychological aspects such as anxiety can impact an elevated heart rate following surgery. Patients who are greater active may exhibit a more rapid recovery and therefore a quicker return to baseline heart rate. Conversely, patients possessing issues during or after surgery may experience a prolonged elevation in heart rate. Understanding these patient-specific variables is crucial for clinicians to evaluate postoperative heart rate and apply appropriate interventions to ensure optimal patient care.
Postoperative Tachycardia
Tachycardia is/can be/presents as a common complication/occurrence/issue in the post anesthesia care unit recovery room. It refers to/describes/indicates a heart rate above/exceeding/greater than 100/120/140 beats per minute bpm. Several factors/A variety of etiologies/Multiple contributors can contribute/lead to/cause tachycardia in the PACU, including/such as/among which are residual anesthetic effects, pain, anxiety, dehydration, hypovolemia, and electrolyte imbalances/disruptions/disturbances. Early identification/Prompt recognition/Detecting tachycardia is crucial/essential/important to ensure/guarantee/facilitate patient safety. Clinicians should/must/are required to monitor heart rate closely and implement/utilize/apply appropriate interventions such as/including/in cases of fluid resuscitation, medications, and addressing underlying causes/factors/origins.
The Autonomic Nervous System and Postoperative Tachycardia
Perioperative tachycardia, a common occurrence during surgical procedures, originates from the interplay between the sympathetic and parasympathetic divisions of the autonomic nervous system. These branches constantly interact physiological processes to maintain homeostasis. During surgery, various factors such as anesthesia administration, surgical stimuli, and emotional stress can precipitate sympathetic activation, leading to an elevation in heart rate. Conversely, parasympathetic activity may diminish, contributing to the overall tachycardia. Understanding this complex interplay is crucial for effective perioperative management and minimizing adverse outcomes.
Perioperative Monitoring Strategies for Detecting Tachycardia
Effective management of tachycardia during the perioperative period involves meticulous monitoring strategies. Clinicians implement a variety of techniques to detect increased heart rates, which can signify underlying conditions.
Continuous electrocardiogram (ECG) monitoring provides real-time visualization of cardiac rhythm and rate. Pulse oximetry can also detect tachycardia by measuring pulse rate alongside oxygen saturation levels. Invasive hemodynamic variables, such as arterial blood pressure and central venous pressure, can provide additional clues about the cardiovascular status.
Rapid detection of tachycardia allows for timely treatments to correct heart rate and prevent potentially life-threatening complications.
Report this page